- Thyroid
- Hashimoto Thyroiditis and Mortality in Patients with Differentiated Thyroid Cancer: The National Epidemiologic Survey of Thyroid Cancer in Korea and Meta-Analysis
-
Injung Yang, Jae Myung Yu, Hye Soo Chung, Yoon Jung Kim, Yong Kyun Roh, Min Kyu Choi, Sung-ho Park, Young Joo Park, Shinje Moon
-
Endocrinol Metab. 2024;39(1):140-151. Published online January 3, 2024
-
DOI: https://doi.org/10.3803/EnM.2023.1748
-
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
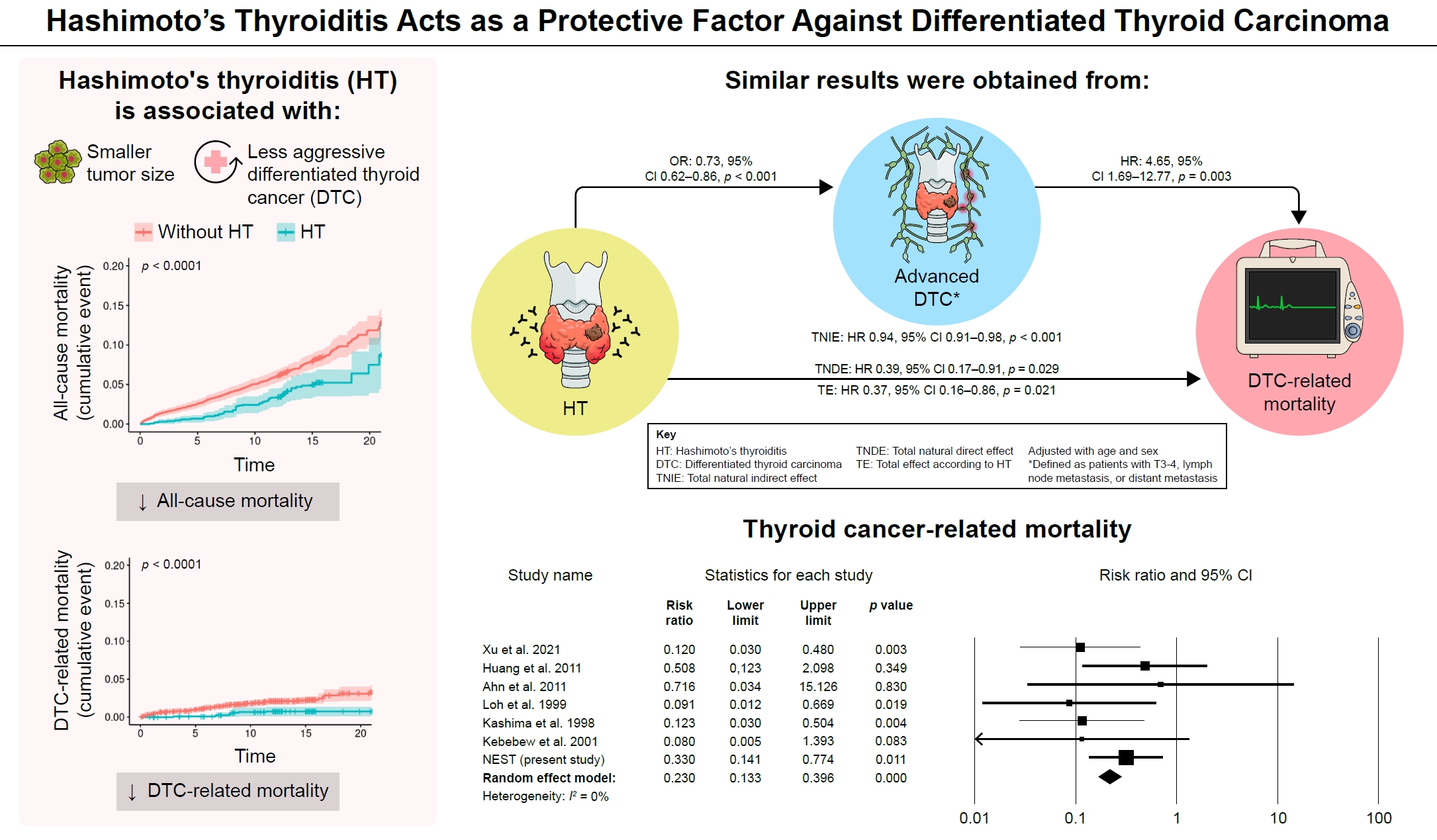
Many studies have shown that Hashimoto’s thyroiditis (HT) acts as a protective factor in differentiated thyroid cancer (DTC), but little is known about its effects on mortality. Therefore, this study was performed to reveal the prognosis of HT on mortality in patients with DTC.
Methods
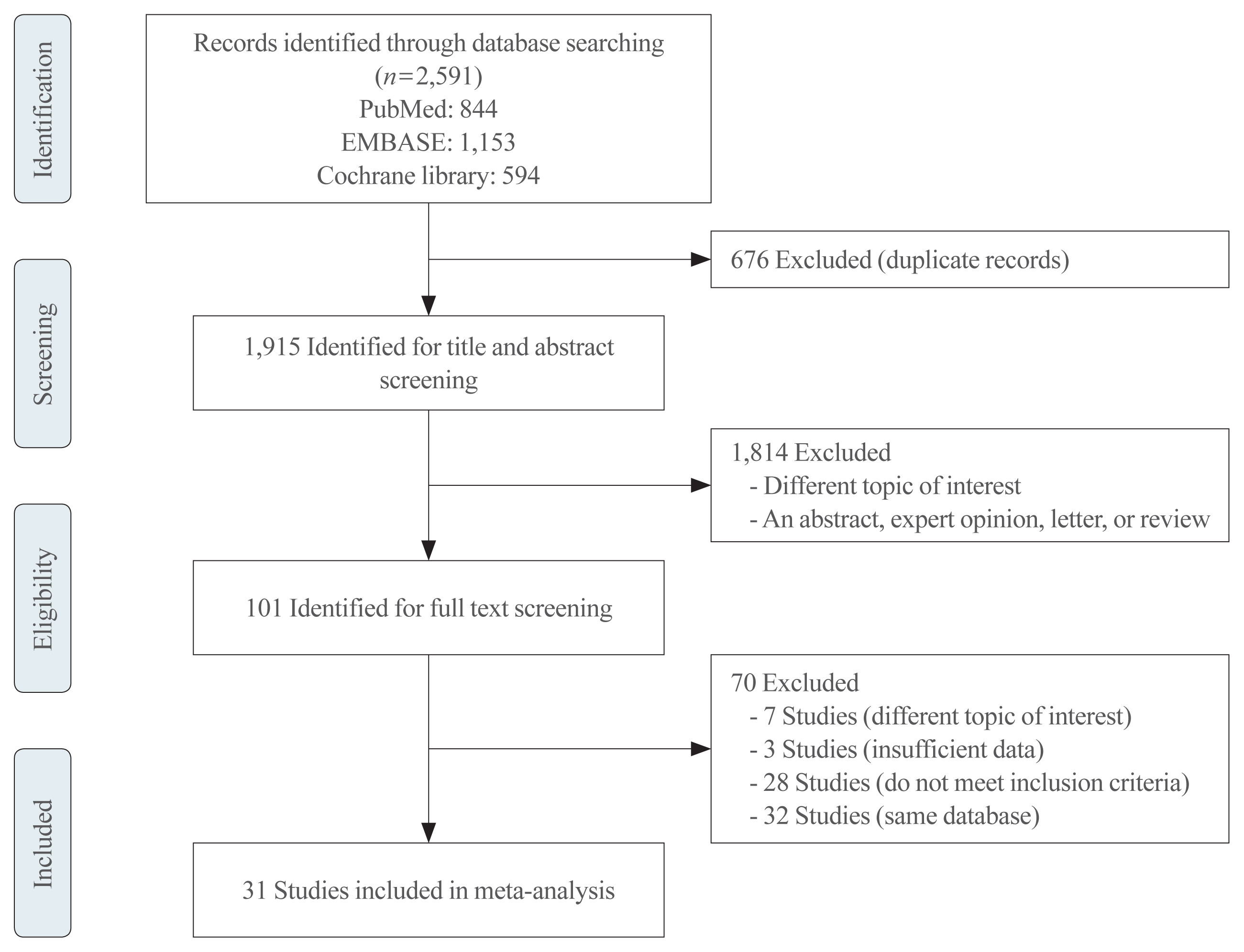
This study included two types of research results: retrospective cohort study using the National Epidemiologic Survey of Thyroid cancer (NEST) in Korea and meta-analysis study with the NEST data and eight selected studies.
Results
Of the 4,398 patients with DTC in NEST, 341 patients (7.8%) died during the median follow-up period of 15 years (interquartile range, 12.3 to 15.6). Of these, 91 deaths (2.1%) were related to DTC. HT was associated with a smaller tumor size and less aggressive DTC. In Cox regression analysis after adjusting for age and sex, patients with HT showed a significantly lower risk of all-cause death (hazard ratio [HR], 0.71; 95% confidence interval [CI], 0.52 to 0.96) and DTC-related death (HR, 0.33; 95% CI, 0.14 to 0.77). The analysis with inverse probability of treatment weight data adjusted for age, sex, and year of thyroid cancer registration showed similar association. The meta-analysis showed that patients with HT showed a lower risk of all-cause mortality (risk ratio [RR], 0.24; 95% CI, 0.13 to 0.47) and thyroid cancer-related mortality (RR, 0.23; 95% CI, 0.13 to 0.40) in comparison with patients without HT.
Conclusion
This study showed that DTC co-presenting with HT is associated with a low risk of advanced DTC and presents a low risk for all-cause and DTC-related death.
- Diabetes, Obesity and Metabolism
- Efficacy and Safety of the New Appetite Suppressant, Liraglutide: A Meta-Analysis of Randomized Controlled Trials
-
Shinje Moon, Jibeom Lee, Hye Soo Chung, Yoon Jung Kim, Jae Myung Yu, Sung Hoon Yu, Chang-Myung Oh
-
Endocrinol Metab. 2021;36(3):647-660. Published online June 18, 2021
-
DOI: https://doi.org/10.3803/EnM.2020.934
-
-
6,203
View
-
302
Download
-
13
Web of Science
-
14
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Obesity is a chronic disease associated with metabolic diseases such as diabetes and cardiovascular disease. Since the U.S. Food and Drug Administration approved liraglutide as an anti-obesity drug for nondiabetic patients in 2014, it has been widely used for weight control in overweight and obese people. This study aimed to systematically analyze the effects of liraglutide on body weight and other cardiometabolic parameters.
Methods
We investigated articles from PubMed, EMBASE, and the Cochrane Library to search randomized clinical trials that examined body weight changes with liraglutide treatment.
Results
We included 31 studies with 8,060 participants for this meta-analysis. The mean difference (MD) between the liraglutide group and the placebo group was −4.19 kg (95% confidence interval [CI], −4.84 to −3.55), with a −4.16% change from the baseline (95% CI, −4.90 to −3.43). Liraglutide treatment correlated with a significantly reduced body mass index (MD: −1.55; 95% CI, −1.76 to −1.34) and waist circumference (MD: −3.11 cm; 95% CI, −3.59 to −2.62) and significantly decreased blood pressure (systolic blood pressure, MD: −2.85 mm Hg; 95% CI, −3.36 to −2.35; diastolic blood pressure, MD: −0.66 mm Hg; 95% CI, −1.02 to −0.30), glycated hemoglobin (MD: −0.40%; 95% CI, −0.49 to −0.31), and low-density lipoprotein cholesterol (MD: –2.91 mg/dL; 95% CI, −5.28 to −0.53; MD: −0.87% change from baseline; 95% CI, −1.17 to −0.56).
Conclusion
Liraglutide is effective for weight control and can be a promising drug for cardiovascular protection in overweight and obese people.
-
Citations
Citations to this article as recorded by  - Pharmacotherapy for obesity: moving towards efficacy improvement
Walmir Coutinho, Bruno Halpern
Diabetology & Metabolic Syndrome.2024;[Epub] CrossRef - Physiopathology and Treatment of Obesity and Overweight: A Proposal for a New Anorectic
Bruno Silvestrini, Mauro Silvestrini, Mayank Choubey
Journal of Obesity.2024; 2024: 1. CrossRef - Side effect profile of pharmacologic therapies for liver fibrosis in nonalcoholic fatty liver disease: a systematic review and network meta-analysis
Yilin Li, Rong Lei, Honglin Lei, Qin Xiong, Fengjiao Xie, Chengjiao Yao, Peimin Feng
European Journal of Gastroenterology & Hepatology.2023; 35(1): 1. CrossRef - Recommendations for the prevention and management of obesity in the Iraqi population
Hussein Ali Nwayyir, Esraa Majid Mutasher, Osama Mohammed Alabid, Muthana Abdulrazzaq Jabbar, Wefak Hasan Abdulraheem Al-Kawaz, Haider Ayad Alidrisi, Majid Alabbood, Muhammed Chabek, Munib AlZubaidi, Lujain Anwar Al-khazrajy, Ibtihal Shukri Abd Alhaleem,
Postgraduate Medicine.2023; 135(5): 425. CrossRef - A Comprehensive Review on Weight Loss Associated with Anti-Diabetic Medications
Fatma Haddad, Ghadeer Dokmak, Maryam Bader, Rafik Karaman
Life.2023; 13(4): 1012. CrossRef - Liraglutide, a glucagon-like peptide-1 analog, in individuals with obesity in clinical practice
Juyoung Shin, Raeun Kim, Hun-Sung Kim
Cardiovascular Prevention and Pharmacotherapy.2023; 5(2): 49. CrossRef - The effects of subcutaneous Tirzepatide on obesity and overweight: a systematic review and meta‐regression analysis of randomized controlled trials
Pejman Rohani, Nasser Malekpour Alamdari, Seyedeh Elaheh Bagheri, Azita Hekmatdoost, Mohammad Hassan Sohouli
Frontiers in Endocrinology.2023;[Epub] CrossRef - Efficacy and safety of liraglutide for weight management in children and adolescents: a systematic review and meta-analysis of randomized controlled trials
Hao Gou, Yiman Zhai, Junjun Guo
European Journal of Pediatrics.2023; 182(11): 5095. CrossRef - Efficacy and safety of once-weekly semaglutide in adults with overweight or obesity: a meta-analysis
Ping Zhong, Hai Zeng, Miaochun Huang, Wenbin Fu, Zhixia Chen
Endocrine.2022; 75(3): 718. CrossRef - Pharmacological profile of once-weekly injectable semaglutide for chronic weight management
David C. W. Lau, Rachel L Batterham, Carel W. le Roux
Expert Review of Clinical Pharmacology.2022; 15(3): 251. CrossRef - Pharmacological Management of Obesity: A Century of Expert Opinions in Cecil Textbook of Medicine
Peter Manu, Cristina-Mihaela Lăcătuşu, Liliana M. Rogozea, Simona Cernea
American Journal of Therapeutics.2022; 29(4): e410. CrossRef - GLP-1 agonists: superior for mind and body in antipsychotic-treated patients?
Katerina Horska, Jana Ruda-Kucerova, Silje Skrede
Trends in Endocrinology & Metabolism.2022; 33(9): 628. CrossRef - Targeting skeletal muscle mitochondrial health in obesity
Chantal A. Pileggi, Breana G. Hooks, Ruth McPherson, Robert R.M. Dent, Mary-Ellen Harper
Clinical Science.2022; 136(14): 1081. CrossRef - A Study on Weight Loss Cause as per the Side Effect of Liraglutide
Jin Yu, Jeongmin Lee, Seung-Hwan Lee, Jae-Hyung Cho, Hun-Sung Kim, Heng Zhou
Cardiovascular Therapeutics.2022; 2022: 1. CrossRef
- Thyroid
- Associations between Hashimoto Thyroiditis and Clinical Outcomes of Papillary Thyroid Cancer: A Meta-Analysis of Observational Studies
-
Shinje Moon, Hye Soo Chung, Jae Myung Yu, Hyung Joon Yoo, Jung Hwan Park, Dong Sun Kim, Young Joo Park
-
Endocrinol Metab. 2018;33(4):473-484. Published online November 30, 2018
-
DOI: https://doi.org/10.3803/EnM.2018.33.4.473
-
-
8,175
View
-
115
Download
-
58
Web of Science
-
55
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Epidemiological studies have suggested an association between Hashimoto thyroiditis (HT) and papillary thyroid cancer (PTC) development. Other studies, however, have reported a protective role of HT against PTC progression. Through this updated meta-analysis, we aimed to clarify the effects of HT on the progression of PTC. MethodsWe searched citation databases, including PubMed and Embase, for relevant studies from inception to September 2017. From these studies, we calculated the pooled odds ratios (ORs) of clinicopathologic features and the relative risk (RR) of PTC recurrence with 95% confidence intervals (CIs) using the Mantel-Haenszel method. Additionally, the Higgins I2 statistic was used to test for heterogeneity. ResultsThe meta-analysis included 71 published studies with 44,034 participants, among whom 11,132 had HT. We observed negative associations between PTC with comorbid HT and extrathyroidal extension (OR, 0.74; 95% CI, 0.68 to 0.81), lymph node metastasis (OR, 0.82; 95% CI, 0.72 to 0.94), distant metastasis (OR, 0.49; 95% CI, 0.32 to 0.76), and recurrence (RR, 0.50; 95% CI, 0.41 to 0.61). ConclusionIn this meta-analysis, PTC patients with HT appeared to exhibit more favorable clinicopathologic characteristics and a better prognosis than those without HT.
-
Citations
Citations to this article as recorded by  - Malignancy risk of indeterminate lymph node at the central compartment in patients with thyroid cancer and concomitant sonographic thyroiditis
Jung Hyo Rhim, Ji Ye Lee, Sun‐Won Park, Younghen Lee, So Lyung Jung, Tae Jin Yun, Eun Ju Ha, Jung Hwan Baek, Jinna Kim, Dong Gyu Na, Ji‐hoon Kim
Head & Neck.2024;[Epub] CrossRef - Hashimoto Thyroiditis and Mortality in Patients with Differentiated Thyroid Cancer: The National Epidemiologic Survey of Thyroid Cancer in Korea and Meta-Analysis
Injung Yang, Jae Myung Yu, Hye Soo Chung, Yoon Jung Kim, Yong Kyun Roh, Min Kyu Choi, Sung-ho Park, Young Joo Park, Shinje Moon
Endocrinology and Metabolism.2024;[Epub] CrossRef - Interaction of BANCR in the relationship between Hashimoto’s thyroiditis and papillary thyroid carcinoma expression patterns and possible molecular mechanisms
Jiabo Zhang, Lingli Yao, Yu Guo
The Journal of Gene Medicine.2024;[Epub] CrossRef - Association between Thyroid Cancer Treatment Outcomes and the Presence of Autoimmune Thyroiditis
Jie Liu
Clinical Thyroidology®.2024; 36(1): 26. CrossRef - Risk prediction for central lymph node metastasis in isolated isthmic papillary thyroid carcinoma by nomogram: A retrospective study from 2010 to 2021
Yu Zhao, Wei Shi, Fang Dong, Xiuhua Wang, Chong Lu, Chunping Liu
Frontiers in Endocrinology.2023;[Epub] CrossRef - The evaluation of locoregional tumoral involvement in the cooccurrence of hashimoto thyroiditis with papillary thyroid cancer: a case controlled study
Shirzad Nasiri, Seyed Mostafa Meshkati Yazd, Mahsa Gholami, Sepehr Shahriarirad, Sina Sharghi, Reza Shahriarirad
BMC Endocrine Disorders.2023;[Epub] CrossRef - Hashimoto’s Thyroiditis: A Protective Factor against Recurrence in BRAF-Wild Type Differentiated Thyroid Carcinoma
Peter P. Issa, Mahmoud Omar, Yusef Buti, Mohamed Aboueisha, Ruhul Munshi, Mohammad Hussein, Muhib Haidari, Graham Blair, Chad P. Issa, Mohamed Shama, Eman Toraih, Emad Kandil
Cancers.2023; 15(8): 2371. CrossRef - VITAMIN D AND AUTOIMMUNE THYROIDITIS
K. V. Pivtorak, O. V Ivanhuk O. V
Bulletin of Problems Biology and Medicine.2023; 1(1): 44. CrossRef - Does the Association of Hashimoto's Thyroiditis with
Differentiated Thyroid Cancer Really Have a Protective Role?
Ahmet Numan Demir, Zehra Kara, Cem Sulu, Serhat Uysal, Serdar Sahin, Guldana Zulfaliyeva, Oznur Aydin Atar, Nahida Valikhanova, Tulin Ozturk, Hande Mefkure Ozkaya, Mustafa Sait Gonen
Hormone and Metabolic Research.2023; 55(06): 388. CrossRef - Ultrasound, laboratory and histopathological insights in diagnosing papillary thyroid carcinoma in a paediatric population: a single centre follow-up study between 2000-2022
Dominika Januś, Małgorzata Wójcik, Anna Taczanowska-Niemczuk, Aleksandra Kiszka-Wiłkojć, Monika Kujdowicz, Małgorzata Czogała, Wojciech Górecki, Jerzy B. Starzyk
Frontiers in Endocrinology.2023;[Epub] CrossRef - Early Post-operative Stimulated Serum Thyroglobulin: Role in Preventing Unnecessary Radioactive Iodine Treatment in Low to Intermediate Risk Papillary Thyroid Cancer
Havva Sezer, Dilek Yazıcı, Tarık Terzioğlu, Serdar Tezelman, Hande Bulut Canbaz, Aslıhan Yerlikaya, Mehmet Onur Demirkol, Yersu Kapran, Bülent Çolakoğlu, Eda Nur Çilingiroğlu, Faruk Alagöl
The American Surgeon™.2023; 89(12): 5996. CrossRef - 2023 Korean Thyroid Association Management Guidelines for Patients with Thyroid Nodules
Young Joo Park, Eun Kyung Lee, Young Shin Song, Soo Hwan Kang, Bon Seok Koo, Sun Wook Kim, Dong Gyu Na, Seung-Kuk Baek, So Won Oh, Min Kyoung Lee, Sang-Woo Lee, Young Ah Lee, Yong Sang Lee, Ji Ye Lee, Dong-Jun Lim, Leehi Joo, Yuh-Seog Jung, Chan Kwon Jung
International Journal of Thyroidology.2023; 16(1): 1. CrossRef - Clonal redemption of B cells in cancer
Tyler R. McCaw, Serena Y. Lofftus, Joseph G. Crompton
Frontiers in Immunology.2023;[Epub] CrossRef - Prevalence and Impact of BRAF mutation in patients with concomitant papillary thyroid carcinoma and Hashimoto’s thyroiditis: a systematic review with meta-analysis
Lukasz Janicki, Agastya Patel, Jarosław Jendrzejewski, Andrzej Hellmann
Frontiers in Endocrinology.2023;[Epub] CrossRef - The role of vascular endothelial growth factor in the development of papillary thyroid carcinoma in patients with lymphocytic thyroiditis
Nese E. GULCELIK, Safak AKIN, Kadriye AYDIN, Cisel AYDIN MERICOZ, Yesim G. GULER TEZEL, Aydan USMAN
Minerva Endocrinology.2023;[Epub] CrossRef - Chronic Lymphocytic Thyroiditis and Aggressiveness of Pediatric Differentiated Thyroid Cancer
Richard M. Yeker, Amber D. Shaffer, Pushpa Viswanathan, Selma F. Witchel, Kevin Mollen, Linwah Yip, Sara E. Monaco, Umamaheswar Duvvuri, Jeffrey P. Simons
The Laryngoscope.2022; 132(8): 1668. CrossRef - Bisphenol A drives di(2-ethylhexyl) phthalate promoting thyroid tumorigenesis via regulating HDAC6/PTEN and c-MYC signaling
Xuan Zhang, Nan Guo, Hao Jin, Renqi Liu, Zhen Zhang, Cheng Cheng, Zhijun Fan, Guopei Zhang, Mingyang Xiao, Shengwen Wu, Yuejiao Zhao, Xiaobo Lu
Journal of Hazardous Materials.2022; 425: 127911. CrossRef - Squamous Differentiation in the Thyroid: Metaplasia, Neoplasia, or Bystander?
Meagan A. Chambers, Peter M. Sadow, Darcy A. Kerr
International Journal of Surgical Pathology.2022; 30(4): 385. CrossRef - Vitamin D Implications and Effect of Supplementation in Endocrine Disorders: Autoimmune Thyroid Disorders (Hashimoto’s Disease and Grave’s Disease), Diabetes Mellitus and Obesity
Dorina Galușca, Mihaela Simona Popoviciu, Emilia Elena Babeș, Mădălina Vidican, Andreea Atena Zaha, Vlad Victor Babeș, Alexandru Daniel Jurca, Dana Carmen Zaha, Florian Bodog
Medicina.2022; 58(2): 194. CrossRef - Central Compartment Lymph Nodes Have Distinct Metastatic Patterns in Different Age Groups
Caigu Yan, Xianghui He, Zuoyu Chen, Yizeng Wang
Frontiers in Endocrinology.2022;[Epub] CrossRef - Synchronous occurrence of papillary thyroid microcarcinoma, medullary thyroid carcinoma and Hashimoto thyroiditis in a single thyroid: A case report with literature review
Ari M. Abdullah, Rawa M. Ali, Karzan M. Salih, Karukh K. Mohammed, Fahmi H. Kakamad, Abdulwahid M. Salih
International Journal of Surgery Case Reports.2022; 93: 106888. CrossRef - Benign and malignant thyroid nodules with autoimmune thyroiditis
Georgia N. Kassi, Catherine C. Evangelopoulou, Konstantinos D. Papapostolou, Helen J. Karga
Archives of Endocrinology and Metabolism.2022;[Epub] CrossRef - Association between Hashimoto thyroiditis and clinical outcomes of papillary thyroid carcinoma: A meta-analysis
Qizhi Tang, Weiyu Pan, Liangyue Peng, Francis Moore
PLOS ONE.2022; 17(6): e0269995. CrossRef - A Narrative Review of Preventive Central Lymph Node Dissection in Patients With Papillary Thyroid Cancer - A Necessity or an Excess
David D. Dolidze, Alexey V. Shabunin, Robert B. Mumladze, Arshak V. Vardanyan, Serghei D. Covantsev, Alexander M. Shulutko, Vasiliy I. Semikov, Khalid M. Isaev, Airazat M. Kazaryan
Frontiers in Oncology.2022;[Epub] CrossRef - Role of papillary thyroid carcinoma patients with Hashimoto thyroiditis: evaluation of oxidative stress and inflammatory markers
Natália Medeiros Dias Lopes, Hannah Hamada Mendonça Lens, Walison Augusto da Silva Brito, Julya Karen Bianchi, Poliana Camila Marinello, Rubens Cecchini, André Armani, Alessandra Lourenço Cecchini
Clinical and Translational Oncology.2022; 24(12): 2366. CrossRef - Emerging trends and hot spots in autoimmune thyroiditis research from 2000 to 2022: A bibliometric analysis
Qiuxian Li, Wanyu Yang, Jiashu Li, Zhongyan Shan
Frontiers in Immunology.2022;[Epub] CrossRef - The Immune Landscape of Papillary Thyroid Cancer in the Context of Autoimmune Thyroiditis
Fabiana Pani, Paola Caria, Yoshinori Yasuda, Miyara Makoto, Stefano Mariotti, Laurence Leenhardt, Solmaz Roshanmehr, Patrizio Caturegli, Camille Buffet
Cancers.2022; 14(17): 4287. CrossRef - Comprehensive analysis of lncRNA-mediated ceRNA regulatory networks and key genes associated with papillary thyroid cancer coexistent with Hashimoto’s thyroiditis
Yuepeng Zhang, Yueli Tian
BMC Endocrine Disorders.2022;[Epub] CrossRef - Elastographic Evaluation of Thyroid Nodules in Children and Adolescents with Hashimoto’s Thyroiditis and Nodular Goiter with Reference to Cytological and/or Histopathological Diagnosis
Hanna Borysewicz-Sańczyk, Beata Sawicka, Filip Bossowski, Janusz Dzięcioł, Artur Bossowski
Journal of Clinical Medicine.2022; 11(21): 6339. CrossRef - Prognostic value of the preoperative and early trends in postoperative serum thyroglobulin antibody levels among patients with papillary thyroid carcinoma and concomitant Hashimoto’s thyroiditis
Siyuan Xu, Hui Huang, Jiaxin Qian, Xiaolei Wang, Zhengang Xu, Shaoyan Liu, Jie Liu
Endocrine.2022; 80(2): 392. CrossRef - What has changed in the last 20 years in the postoperative specimen findings of the papillary thyroid cancer cases? A retrospective analysis
Burak Bakar, Pınar Taşar, Turkay Kırdak, Sadık Kılıçturgay
Turkish Journal of Surgery.2022; 38(4): 345. CrossRef - A nomogram model based on the preoperative clinical characteristics of papillary thyroid carcinoma with Hashimoto's thyroiditis to predict central lymph node metastasis
Wanjun Zhao, Linye He, Jingqiang Zhu, Anping Su
Clinical Endocrinology.2021; 94(2): 310. CrossRef - The Association of Histologically Proven Chronic Lymphocytic Thyroiditis with Clinicopathological Features, Lymph Node Metastasis, and Recurrence Rates of Differentiated Thyroid Cancer
Berna İmge Aydoğan, Adile Begüm Bahçecioğlu Mutlu, Seher Yüksel, Sevim Güllü, Rıfat Emral, Özgür Demir, Mustafa Şahin, Vedia Tonyukuk Gedik, Demet Çorapçıoğlu, Serpil Dizbay Sak, Murat Faik Erdoğan
Endocrine Pathology.2021; 32(2): 280. CrossRef - Beneficial autoimmunity improves cancer prognosis
Laurence Zitvogel, Claude Perreault, Olivera J. Finn, Guido Kroemer
Nature Reviews Clinical Oncology.2021; 18(9): 591. CrossRef - Influence Factors for Lymph Node Metastasis in Papillary Thyroid Carcinoma: Hashimoto’s Thyroiditis Has a Weak Effect on Central or Lateral Lymph Node Metastasis
Liguang Zhou, Gang Chen, Lei Sheng, Nan Liu, Bin Zhang, Qingdong Zeng, Bo Chen
Cancer Management and Research.2021; Volume 13: 3953. CrossRef - Implications of a background of Hashimoto’s thyroiditis on the current conservative surgical trend towards papillary thyroid carcinoma
Shadi Hamouri, Sohail Bakkar, Almoutuz Aljaafreh, Mohammed Bani Hani, Hussein Heis, Ghazi Qasaimeh, Nasr Alrabadi, Wisam Al Gargaz, Haitham Odat, Yazan Alkurdi, Tarek Manasreh, Mohammad Matalka, Moamin Badwan
Updates in Surgery.2021; 73(5): 1931. CrossRef - Thyroid nodules in childhood‐onset Hashimoto's thyroiditis: Frequency, risk factors, follow‐up course and genetic alterations of thyroid cancer
Yun Jeong Lee, Yeon Jin Cho, You Joung Heo, Eun‐Jae Chung, Young Hun Choi, Jong‐Il Kim, Young Joo Park, Choong Ho Shin, Young Ah Lee
Clinical Endocrinology.2021; 95(4): 638. CrossRef - Prevalence of Hashimoto Thyroiditis in Adults With Papillary Thyroid Cancer and Its Association With Cancer Recurrence and Outcomes
Siyuan Xu, Hui Huang, Jiaxin Qian, Yang Liu, Ying Huang, Xiaolei Wang, Shaoyan Liu, Zhengang Xu, Jie Liu
JAMA Network Open.2021; 4(7): e2118526. CrossRef - The Effects of Chronic Lymphocytic Thyroiditis on Clinicopathologic Factors in Papillary Thyroid Cancer
Davut Sakiz, Muhammed Erkam Sencar, Murat Calapkulu, Ilknur Ozturk Unsal, Levent Aktas, Bekir Ucan, Mustafa Ozbek, Erman Cakal
Endocrine Practice.2021; 27(12): 1199. CrossRef - Significance of DMBT1 in Papillary Thyroid Carcinoma Concurrent With Hashimoto’s Thyroiditis
Xiao-xiong Gan, Ya-yi Li, Si-jin Li, Shi-sen Mo, Jian-hua Feng, Fei Shen, Wen-song Cai, Ye-qian Lai, Bo Xu
Frontiers in Oncology.2021;[Epub] CrossRef - Pre-existing Thyroiditis Ameliorates Papillary Thyroid Cancer: Insights From a New Mouse Model
Fabiana Pani, Yoshinori Yasuda, Giulia Di Dalmazi, Paulina Chalan, Kathleen Gabrielson, Luigi Adamo, Elena Sabini, Stefano Mariotti, Patrizio Caturegli
Endocrinology.2021;[Epub] CrossRef - Autoimmunity affecting the biliary tract fuels the immunosurveillance of cholangiocarcinoma
Juliette Paillet, Céleste Plantureux, Sarah Lévesque, Julie Le Naour, Gautier Stoll, Allan Sauvat, Pamela Caudana, Jimena Tosello Boari, Norma Bloy, Sylvie Lachkar, Isabelle Martins, Paule Opolon, Andrea Checcoli, Agathe Delaune, Noémie Robil, Pierre de l
Journal of Experimental Medicine.2021;[Epub] CrossRef - Papillary Thyroid Cancer Prognosis: An Evolving Field
Salvatore Ulisse, Enke Baldini, Augusto Lauro, Daniele Pironi, Domenico Tripodi, Eleonora Lori, Iulia Catalina Ferent, Maria Ida Amabile, Antonio Catania, Filippo Maria Di Matteo, Flavio Forte, Alberto Santoro, Piergaspare Palumbo, Vito D’Andrea, Salvator
Cancers.2021; 13(21): 5567. CrossRef - Overexpression of PD-L1 in Papillary Carcinoma and Its Association with Clinicopathological Variables
Servet KOCAÖZ, Gülay TURAN
Düzce Tıp Fakültesi Dergisi.2021; 23(3): 252. CrossRef - Correlation Between Hashimoto's Thyroiditis–Related Thyroid Hormone Levels and 25-Hydroxyvitamin D
Guanqun Chao, Yue Zhu, Lizheng Fang
Frontiers in Endocrinology.2020;[Epub] CrossRef - Oncological impact of hypothyroidism and levothyroxine supplementation following hemithyroidectomy in patients with papillary thyroid carcinoma
Dongbin Ahn, Gil J. Lee, Jin H. Sohn, Jae H. Jeon
Head & Neck.2020; 42(5): 1004. CrossRef - Suspicious ultrasound characteristics correlate with multiple factors that predict central lymph node metastasis of papillary thyroid carcinoma: Significant role of HBME-1
Li Jianming, Liu Jibin, Qian Linxue
European Journal of Radiology.2020; 123: 108801. CrossRef - Unexpected high‐risk pathologic features following thyroidectomy in the chinese immigrant population
Arvind K. Badhey, Erin Moshier, Ameya Jategaonkar, Anni Wong, Kristen Echanique, Raymond L. Chai
The Laryngoscope.2020; 130(7): 1844. CrossRef - Hashimoto's thyroiditis attenuates progression of papillary thyroid carcinoma: deciphering immunological links
Oksana Sulaieva, Oleksii Selezniov, Dmytro Shapochka, Nataliia Belemets, Oleksandr Nechay, Yelizaveta Chereshneva, Dibakhan Tsomartova, Marina Ivanova
Heliyon.2020; 6(1): e03077. CrossRef - Changes in Treg numbers and activity in papillary thyroid carcinoma with and without Hashimoto’s thyroiditis
Na Zhao, Xin Liu, Chao Wu, Yuanchao Liu, Xiangnan Zhao, Xianghui He
Journal of International Medical Research.2020; 48(4): 030006052091922. CrossRef - Genetic relationship between Hashimoto`s thyroiditis and papillary thyroid carcinoma with coexisting Hashimoto`s thyroiditis
Ohoud Subhi, Hans-Juergen Schulten, Nadia Bagatian, Roa'a Al-Dayini, Sajjad Karim, Sherin Bakhashab, Reem Alotibi, Alaa Al-Ahmadi, Manar Ata, Aisha Elaimi, Saad Al-Muhayawi, Majid Mansouri, Khalid Al-Ghamdi, Osman Abdel Hamour, Awatif Jamal, Jaudah Al-Mag
PLOS ONE.2020; 15(6): e0234566. CrossRef - Hashimoto's thyroiditis as a risk factor for thyroid cancer
Ulla Feldt-Rasmussen
Current Opinion in Endocrinology, Diabetes & Obesity.2020; 27(5): 364. CrossRef - Predictive Factors of Recurrence for Multifocal Papillary Thyroid Microcarcinoma With Brafv600e Mutation: A Single Center Study of 1,207 Chinese Patients
Shuai Xue, Li Zhang, Peisong Wang, Jia Liu, Yue Yin, Meishan Jin, Liang Guo, Yuhua Zhou, Guang Chen
Frontiers in Endocrinology.2019;[Epub] CrossRef - Hashimotos’ thyroiditis: Epidemiology, pathogenesis, clinic and therapy
Francesca Ragusa, Poupak Fallahi, Giusy Elia, Debora Gonnella, Sabrina Rosaria Paparo, Claudia Giusti, Leonid P. Churilov, Silvia Martina Ferrari, Alessandro Antonelli
Best Practice & Research Clinical Endocrinology & Metabolism.2019; 33(6): 101367. CrossRef - Características anatomopatológicas del carcinoma papilar de tiroides en especimenes con y sin tiroiditis linfocitica crónica.
Carlos Osorio Covo, Jorge Ballestas Barrera, Jorge Martínez Castro, Zully Acevedo Meza, Diego Barrios Castellar, Francisco Herrera Sáenz, Cesar Redondo Bermúdez, Katherine Redondo De Oro
Revista Ciencias Biomédicas.2019; 8(2): 32. CrossRef
- Sustained Maintenance of Normal Insulin-like Growth Factor-I during Pregnancy and Successful Delivery in an Acromegalic Patient with Octreotide-LAR(R) Treatment.
-
Soo Kyoung Kim, Jung Hwa Jung, Jae Hyeon Kim, Kyu Yeon Hur, Alice Hyun Tan, Hee Kyung Kim, Ji In Lee, Hye Soo Chung, Kwang Won Kim
-
Endocrinol Metab. 2010;25(3):213-216. Published online September 1, 2010
-
DOI: https://doi.org/10.3803/EnM.2010.25.3.213
-
-
 Abstract Abstract
 PDF PDF
- We report here on a 34-year-old Korean woman with active acromegaly and who received Octreotide-LAR(R) for 12 months following transsphenoidal pituitary surgery. During Octreotide-LAR(R) treatment, the clinical improvement was paralleled with the decrease of the growth hormone levels to 1.1 ng/mL and the insulin-like growth factor-I (IGF-I) levels to 345.5 ng/mL. Octreotide-LAR(R) was discontinued when the patient was found to be at the 12th week of pregnancy. During pregnancy, the patient experienced clinical well-being and she maintained her IGF-I levels within the normal range for her age-matched despite discontinuation of Octreotide-LAR(R) treatment at early gestation. She delivered a full-term healthy male infant. The serum IGF-I levels of the patient increased progressively increased after delivery. This report describes a successful pregnancy in an acromegalic woman who was exposed to Octreotide-LAR(R) during the early gestational period. She and who showed an unexpected pattern of persistently normal IGF-I levels through the pregnancy despite discontinuation of Octreotide-LAR(R) therapy.
- Two Cases of Acromegaly with Empty Sella Syndrome Treated by Long-Acting Release Octreotide.
-
Dong Jin Kim, Young Jin Seo, Nam Hoon Kim, Hye Soo Chung, Chai Ryoung Eun, Hye Jung Choi, Hye Sook Kim, Sae Jeong Yang, Juri Park, Hye Jin Yoo, Soo Yeon Park, Yun Jeong Lee, Ohk Hyun Ryu, Kye Won Lee, Hee Young Kim, Ji A Seo, Sin Gon Kim, Nan Hee Kim, Kyung Mook Choi, Sei Hyun Baik, Dong Seop Choi
-
J Korean Endocr Soc. 2007;22(2):135-141. Published online April 1, 2007
-
DOI: https://doi.org/10.3803/jkes.2007.22.2.135
-
-
 Abstract Abstract
 PDF PDF
- Two cases of typical acromegaly with empty sella syndrome presented to our institution. In the natural course of untreated pituitary adenoma, empty sella syndrome may result from necrosis by infarction or from hemorrhage of the pituitary gland. In our patients, the secretion of growth hormone continued in spite of the existence of empty sella syndrome. In one case, we confirmed the hypersecretion of growth hormone from sella by jugular vein sampling. Medical therapy with somatostatin analogue was attempted because there was no obvious mass in the sella. After 6~12 months of treatment with long-acting release octreotide, clinical features in our patients were improved, and the level of growth hormone and IGF-1 were also normalized.
|